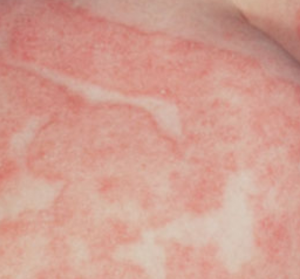
Eczema can be red, blistering, or oozing, it’s not just another itchy rash. The 2 square yards of skin that covers the average adult is constantly exposed to the elements and therefore is susceptible to a variety of problems.
Dermatitis, also called eczema, is an inflammation of the skin. It can have many causes and occur in many types. Generally, dermatitis involves swollen, reddened and itchy skin.
Dermatitis is common, not life-threatening and not contagious. But it can make you feel uncomfortable and self-conscious. A combination of self-care steps and medications can help you treat dermatitis and its symptoms.
Dermatitis occurs in several types, each with distinct signs and symptoms:
- Contact dermatitis. This type of dermatitis occurs with an allergen such as poison ivy or an irritant such as skin soap. Signs and symptoms include redness and itching. In severe cases, you may have blisters and weeping sores. The skin changes in contact dermatitis are limited to where you had contact with the allergen or irritant.
- Neurodermatitis. This type, which occurs because of repeated scratching, may appear as small, flat areas (plaques) of various sizes, 1 to 10 inches (2.5 to 25 centimeters) in diameter. These areas have definite margins that have become thick and leatherlike (lichenified). This type of dermatitis is also known as lichen simplex chronicus.
- Eczema / Seborrheic dermatitis. You may notice greasy, scaling areas at the sides of your nose, between your eyebrows, behind your ears or over your breastbone. This type can appear as a stubborn, itchy dandruff. Dandruff is usually due to mild seborrheic dermatitis of the scalp. Seborrheic dermatitis may appear as cradle cap — crusty, scaly skin on your baby’s scalp. Cradle cap usually doesn’t appear in children older than 1 year.
- Stasis dermatitis. This type often occurs with varicose veins. Stasis dermatitis may cause the skin at your ankles and over your shins to become discolored (red or brown), thick and itchy.
- Atopic dermatitis. Signs and symptoms of this type include itchy, thickened, fissured skin, most often in the folds of the elbows or backs of your knees. When this type occurs in babies, it’s called infantile eczema.
Causes of Eczema
A number of health conditions, allergies, genetic factors, physical and mental stress, and irritants can cause dermatitis.
- Contact dermatitis results from direct contact with one of many irritants or allergens. Common irritants include laundry soap, skin soap and cleaning products. Possible allergens include rubber, metals, jewelry, perfume, cosmetics and weeds such as poison ivy. It takes a larger amount of an irritant over a longer time to cause dermatitis than it takes for an allergen. If you’re sensitized to an allergen, just brief exposure to a small amount of it can cause dermatitis.
- Eczema / Neurodermatitis can occur when something such as a tight garment rubs or scratches your skin. This irritation may lead you to rub or scratch your skin repeatedly. Common locations include ankles, wrist, outer forearm or arm, and the back of your neck.
- Eczema / Seborrheic dermatitis is often an inherited tendency. It may occur during times of stress or in people who have neurologic conditions such as Parkinson’s disease.
Eczema / Stasis dermatitis can occur when fluid accumulates in the tissues just beneath your skin. Varicose veins and other chronic conditions in your legs can cause the fluid buildup. - Atopic dermatitis often occurs with allergies and frequently runs in families in which other family members have asthma or hay fever. It usually begins in infancy and may increase and decrease in severity during childhood and adolescence. It tends to become less of a problem in adulthood, unless you’re exposed to allergens or irritants in the workplace.
Prevention of Eczema
Preventing contact dermatitis means avoiding coming into contact with those substances, such as poison ivy or harsh soaps, that may cause it.
Avoiding dry skin may be one factor in helping you prevent future bouts of dermatitis. These tips can help you minimize the drying effects of bathing on your skin:
- Bathe less frequently. Two or three times a week is often enough for most people. Limit yourself to 15 minutes, and use warm, rather than hot, water.
- Use only certain soaps. Choose superfatted, nonsudsing soaps such as Dove, Basis or Ivory that clean without removing natural oils. Soap substitutes in bar, gel and liquid forms are less drying than deodorant and antibacterial soaps. Use soap only on your face, underarms, genital areas, hands and feet. Use clear water elsewhere.
- Dry yourself carefully. Brush your skin rapidly with the palms of your hands, or gently pat your skin dry with a towel after bathing.
- Moisturize your skin. Seal in moisture, while your skin is still damp, with an oil or cream. Pay special attention to your legs, arms, back and the sides of your body. If your skin is already dry, consider using a lubricating cream such as Vanicream or Eucerin.
Eczema Treatment
Treatment of dermatitis varies, depending on the cause:
- Contact dermatitis. Treatment consists primarily of identifying the cause of irritation and avoiding it. Sometimes, creams containing hydrocortisone, or wet dressings that provide moisture to your skin, may help relieve redness and itching.
- Neurodermatitis. Getting you to stop scratching and to avoid aggravating your skin are the treatment objectives. Accomplishing this may mean wearing a dressing that’s difficult to remove and that’s left on for a week or more. Hydrocortisone lotions and creams may help soothe your skin. You may find that wet compresses provide relief. Sedatives and tranquilizers also may help you stop scratching, but your doctor will want to monitor your use of these substances because they can be addictive.
- Seborrheic dermatitis. You’ll need to frequently shampoo, then carefully rinse your scalp. Your doctor may recommend a specific shampoo. Commonly used shampoos contain tar, zinc pyrithione, salicylic acid or ketoconazole as the active ingredient. Hydrocortisone creams and lotions may soothe your skin and relieve itching. You also may need treatment for a secondary infection.
- Stasis dermatitis. Treatment consists of correcting the condition that causes fluid to accumulate in your ankles for extended periods. This may mean wearing elastic support hose or even choosing varicose vein surgery. You may also use wet dressings to soften the thickened, yet fragile, skin and to control infection.
- Atopic dermatitis. Treatment typically consists of applying hydrocortisone-containing lotions. Two recently approved topical medications are tacrolimus (Protopic) and pimecrolimus (Elidel), medications that affect the immune system. Doctors may recommend using these medications in conjunction with hydrocortisone preparations or in place of them. If your skin cracks open, doctors sometimes prescribe wet dressings with mildly astringent properties that contract the skin and reduce secretions to prevent infection. If itching is severe, your doctor may suggest you take antihistamines.
For all types of dermatitis, occasional use of over-the-counter antihistamines can reduce itching. However what follows is a link that provides documentation to what we believe to be a safe and effective natural alternative to treating and prevention from developing eczema. Internal Natural Alternative.
These links will redirect you to…
Crohn’s Disease and Living Probiotics
Diseases & Illnesses A to Z